This episode is not meant to be a long one, but as I tried to keep it as short as possible, I kept adding a little here, and a little there. I wanted to touch on Epsom salts, SIBO - Small intestinal bacterial overgrowth, IBS - Irritable Bowel Syndrome, Fasting, and the migrating motor complex.
Some people may not be aware but our body has this built-in mechanism called the Migrating Motor Complex that is only triggered when you are in a fasted state for around 4 hours. This mechanism has 4 phases and some people get theirs activated a little earlier, some a little later, and others very infrequently (Think IBS and SIBO sufferers).
You need this migrating motor complex to keep your body functioning optimally. It's just one of many processes that need to function to keep your machine well-oiled. Once it starts to fall apart, you can expect lots of downstream problems as well. I believe that a lot of autoimmune diseases that affect the gut also affect the MMC and therefore fixing this is one of the keys to returning your health.
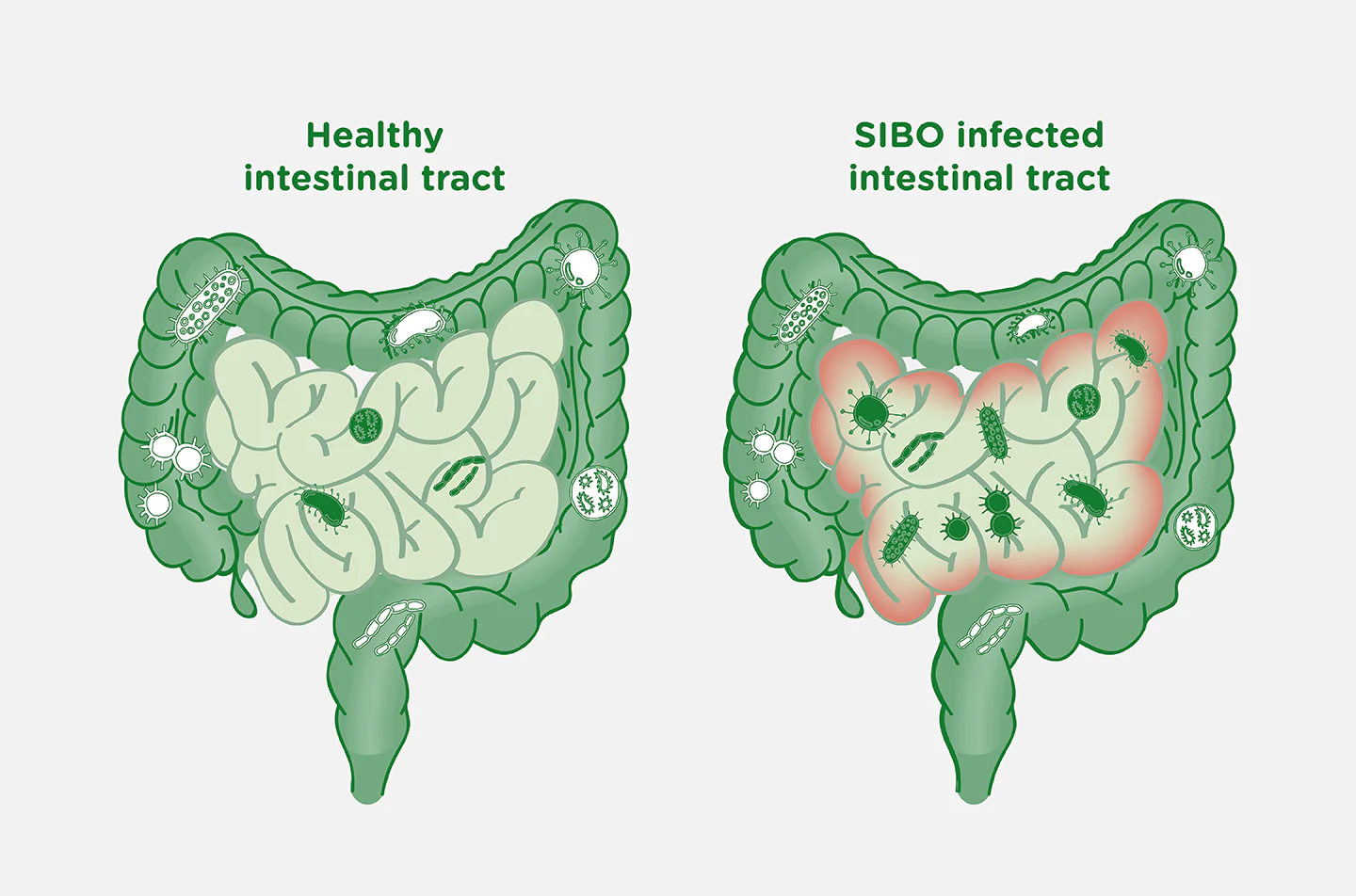
I believe we can all agree that having a cleaner intestinal tract, as opposed to one filled with pathogens, bacteria, and parasites, is better. I mean there are hundreds of parasite cleanses, liver flushes, and more dedicated specifically to this topic.
What blows my mind is how many people try dozens of different cleanses, yet run away from the most effective one: FASTING.
Just understanding that the Migrating motor complex is activated by fasting should be a lightbulb moment for you.
So the digestive system, when it comes to the migrating motor complex and motility kind of boils down to 5 main areas that the food passes through: the mouth, the esophagus, the stomach, the small intestine, and the large intestine.
What is the Migrating Motor Complex?
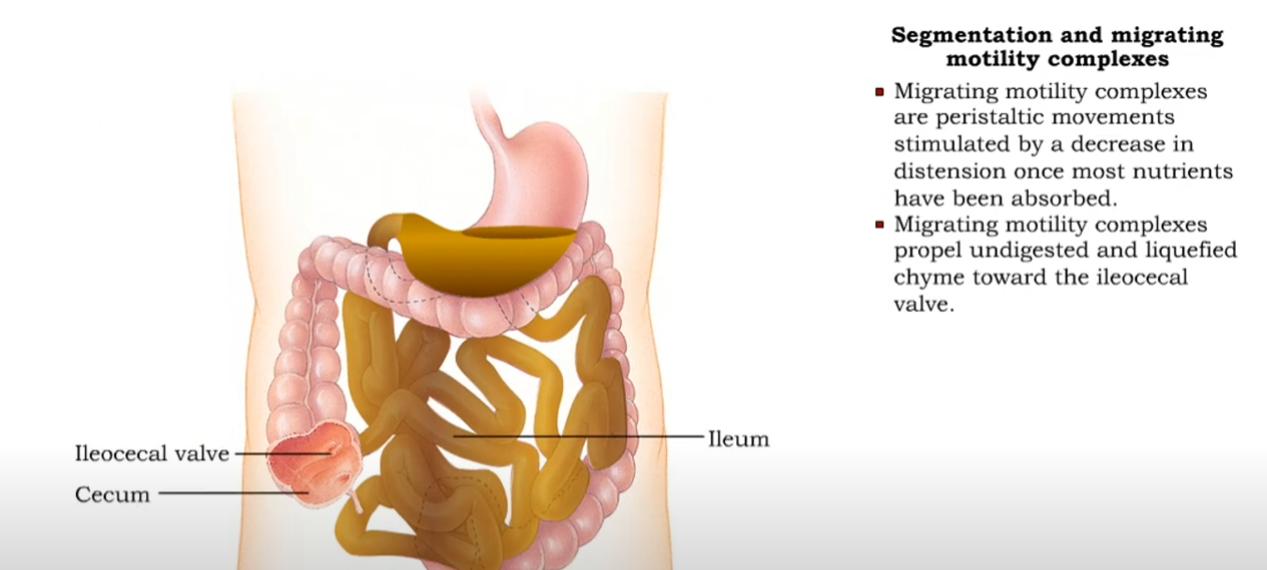
Think of it like the cleaner in the small intestine. The main purpose is to clean the bacteria out of the small intestine. Moving them into the large intestine and eventually to the ileocecal valve and then the colon.
The MMC is what is actually the cleaner and pusher. Without it, you’re really going to struggle with cleaning the small intestine from bacterial overgrowth. Think of it like washing the dishes after a meal. It’s called the digestive system house cleaner wave for a reason.
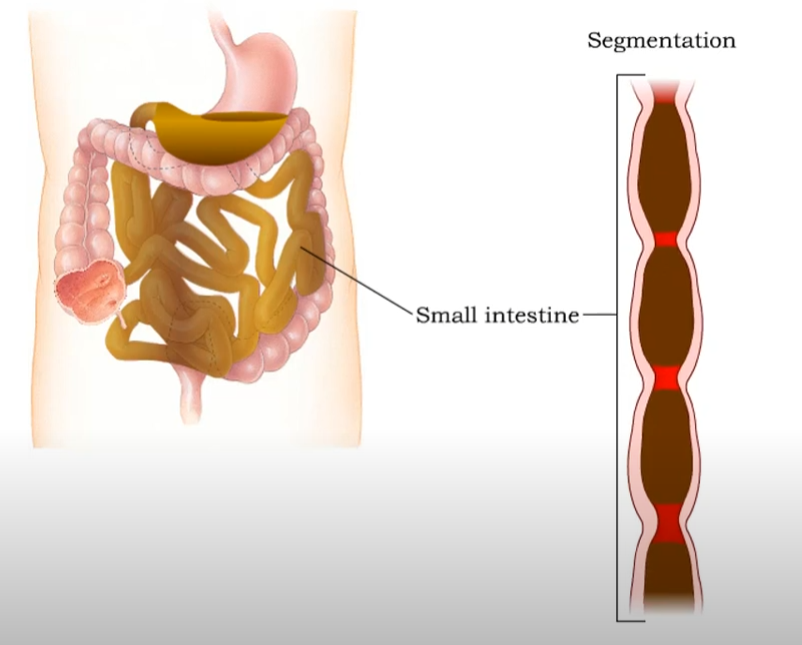
Once again, this only occurs when we are fasting. Peristalsis is occurring at all times. So think of the MMC as the big kahuna, whereas peristalsis is the ongoing small pulse of motility kind of like an energizer bunny. This is so important to consider because it provides further proof that we are not meant to be a constantly snacking species. Fasting is so important. Eating turns off the Migrating motor complex. The exact amount of food is still unknown as everyone is different.
Think that's hunger causing your stomach to rumble? Think again. It's actually your migrating motor complex starting to rev up. And here we think you need to eat something. Yes, eating may stop the rumbling, but at the cost of worse intestinal cleansing.
How does Migratory muscle complex damage usually happen?
Sometimes, harmful bacteria such as E. coli or Salmonella can cause an infection in your gut. When this happens, these bacteria produce a toxin called CDT. Your immune system responds by producing antibodies to fight off this toxin. Commonly this means you get post-infectious damage to the MMC as a result of bacterial infection (e.g. Campylobacter jejuni, E.coli, Shigella, Salmonella)
However, due to an error by the immune system, these antibodies can mistakenly target a protein called vinculin, which is found in certain cells in your gut that are essential for the function of the MMC. When this mistake happens, it can cause permanent damage to the MMC, leading to problems with digestion. This can predispose you to develop Small Intestinal Bacterial Overgrowth (SIBO) or Irritable Bowel Syndrome (IBS). These conditions can occur due to an overactive immune response, also known as an autoimmune response.
We return full circle to autoimmune diseases, something that is rapidly increasing in society. What is the number one remedy for autoimmune diseases? Dry fasting.
Factors that can further damage the MMC
- Impaired sugar metabolism: Unstable blood sugar levels, common in conditions like insulin resistance or hyperglycemia, can influence the normal functioning of the MMC. This is because insulin and glucose levels can affect the hormonal regulation of gut motility.
- Hypothyroidism: This condition can slow down the gut motility, including the MMC. Hypothyroidism often leads to delayed gastric emptying and decreased intestinal motility, which can result in constipation.
- Neurodegenerative diseases: Conditions like multiple sclerosis or Parkinson’s disease can affect the nerves controlling gut motility, thereby impairing MMC function.
- Head injuries: Trauma to the head could potentially impact the brain-gut axis, a communication network between the brain and the gut, thereby potentially interfering with MMC activity.
- Chronic use of certain medications: Prolonged use of medications such as Proton Pump Inhibitors (PPIs), antibiotics, steroids, and hormonal contraceptives can disrupt the gut's microbiota and normal motility, including the MMC.
- Parasitic infections: Parasites can cause inflammation and disrupt the normal functioning of the gut, which may interfere with the MMC.
- Lyme disease, and Yersiniosis: These infectious diseases can affect the nervous system, including the nerves controlling gut motility, thereby potentially interfering with MMC function.
- Celiac disease: This autoimmune disorder damages the small intestine lining, potentially disrupting gut motility, including the MMC.
- Vagus nerve dysfunction: The vagus nerve plays a crucial role in regulating gut motility. If its function is compromised, this can directly impact the MMC.
- Eating disorders: Conditions such as anorexia nervosa can slow gastric emptying and intestinal transit time, potentially interfering with the MMC.
- Long-term stress: Both physical and mental stress can impact the gut-brain axis and hormone production, which can disrupt normal gut motility, including the MMC.
Why does not eating before bed make sense
Now we start to connect the dots.
There’s a reason that we’re always told to not eat before bed.
Well, quantifying it would mean don’t eat around 4 hours before bed, so that your MMC is fully activated before you even sleep, allowing your body to focus on healing and not sending energy and immune cells to combat the food fermenting in your intestines.
Don't forget that when you have digestive issues caused by trauma, bacterial overgrowth, insufficient lymph filtering, or diseases like Covid, your MMC may need even longer to activate.
There’s a reason holistic experts see huge improvements in their patient's health when they don’t eat before bed. Intermittent fasters love to skip breakfast as well, this further continues the MMC waves for a longer period of time, meaning you are getting even better cleaning of the digestive system.
In a perfect world, you would eat meals spaced out by at least 4 hours with no snacking in between. Some people do this with a two-meal 6-hour window approach. It’s my personal favorite. I eat lunch at 12 noon and dinner around 6 PM.
It’s sometimes important to switch things up because the body adapts to routines and to maximize the benefits of hormesis, you need to keep your body guessing. Hormesis and making sure your body does not adapt too well to a certain stressor is another topic that is mentioned in other posts. Look for the Scorch protocol.
This is further evidence as to why things like a low FODMAP diet, and also a carnivore diet seems to help people with gut issues so drastically. You eat less often because you feel full - and this helps you trigger more MMC waves because you are fasting in between meals. I don't want to get down the rabbit hole of microbiome gut bacteria and avoiding fiber, but there's a post about butyrate and the carnivore diet you can check out.
FODMAP Diet, Carnivore Diet, and Autoimmune diseases
Take a look at FODMAP diets. FODMAP stands for fermentable oligosaccharides, disaccharides, monosaccharides, and polyols, which are short-chain carbohydrates (sugars) that the small intestine absorbs poorly. Some people experience digestive distress after eating them.

You may notice that the FODMAP diet has close similarities to the carnivore diet. What does this mean?! Well, for starters, like I've been saying for years now, the carnivore diet should be used as a tool for health.
Think of it like a temporary solution on your journey to actual health. I don't want to go down the rabbit hole of too much protein which leads towards too high mTor activation, which leads to accelerated aging.
I state over and over, carnivore is fantastic for dealing with gut issues, which also affect things like autoimmune diseases, but only in the short term. Yes, it will make you lose fat and gain muscle, but at the cost of your longevity. We're not even talking about the imbalance of electrolytes and the downward spiral of your body having to deal with buffering acidity for too long.
If some of you are saying 'Hah! I always told those carnivores to go vegan" then sit back down, because that is not what I am saying, and you're also not aware that meat and animal-based fat are the best tools and sources of deuterium-depleted water for your body. Lowest form of pesticide foods too, when you take into consideration the average diet. My goal for anyone on the FODMAP diet is to get you to the point where you can eat cups of raw cabbage and feel great. Only then do we know that you are on the right path. There is also no doubt that some of the best, most nutrient dense foods are animal based. However, the key is balance, and finding the right one is important.
Prokinetics: LDN and more
Because we're talking about the Migrating motor complex, I'd be remiss if I didn't bring up prokinetics. Prokinetic agents are drugs that stimulate or regulate muscle contractions in the gastrointestinal (GI) tract, thereby improving the movement of contents through the stomach and intestines. They are often used to treat conditions like gastroparesis, GERD, or constipation.
Prokinetics are meant not just to stimulate motility, but in a coordinated fashion -> make sure motility is going the right way. For example, acid reflux is an example of motility that goes the wrong way. When it comes to SIBO you need a prokinetic that focuses on motility in the small intestine.
Difference between laxatives and prokinetics
A Prokinetic CAN be a Laxative. But most laxatives are NOT prokinetics. For example, an osmotic laxative can be magnesium or vitamin C.
Both of these are osmotic because they draw water into the large intestine, which fluffs up the stool and helps it move through the bowels. Some people think they take magnesium so they don’t need a prokinetic… a little silly but a popular assumption to make.
Specifically with fasting, and preparing for extended fasts, we use magnesium sulfate to help flush the bowels. But this is a hyperosmotic laxative that helps with gallbladder contraction, so in essence, it plays a key role in liver and gallbladder flushing. If you want to take it one step further you add the oil and citrus to stimulate a bile flush as well, but that goes outside the scope of this topic. Look up the post about dry fasting and intestinal cleanses.
Dry fasting stimulates the Migratory muscle complex, so no need for prokinetics if you’re dry fasting, but both pre and post-fast ginger is a critical health-boosting component that can also double as nature’s prokinetic.
This also explains why dry fasting and fasting, in general, is a critical key to curing long covid. This also explains why LDN helps so much in the FLCCC protocol. They may not make the connections to the MMC but if you are aware of these connections it really starts to make a lot of sense.
The FLCCC, Long Covid, and Low-dose Naltrexone
I definitely jump around topics a little much and there's so much to say, but unfortunately, so little time. Low-dose naltrexone is a first-line therapy in the FLCCC protocol. For Long Covid Recovery the FLCCC has built a protocol that is probably the most popular recovery protocol.
If you haven’t heard of the FLCCC you’re either a new long hauler, lived under a rock, never had covid complications, or you tune out when you hear the word ivermectin. My advice to you is not to discount it.
The FLCCC uses it in its protocol. It includes ivermectin at 0.2mg/kg body weight for a week, prednisone as a corticosteroid 10-15mg, and low-dose naltrexone.
Low-dose Naltrexone is an off-label use of naltrexone for its immunomodulatory effects. Naltrexone is actually a drug that is used to treat opioid addiction. Think Heroin addicts. LDN or low-dose naltrexone is about 1/10th the power of the actual opioid addiction treatment dosage. The mechanism of action of Low-dose naltrexone is not greatly understood but one of the mechanisms includes blocking of opioid receptors and therefore increasing endorphin production.

When it comes to SIBO, and you have a chronic case of IBS, you may have to be on LDN for 3-6 months. Sometimes even long-term, ongoing for 10 years. If you don’t want to become a slave to LDN or other prokinetics when it comes to SIBO/IBS and Migrating motor complex, then dry fasting is your cure.
Every prokinetic has different mechanisms of action. Sometimes it may be beneficial to take two at once.
Ginger and peppermint oil are very popular. Ginger is overall very good for you, and I like to add it to my celery juicing. It just covers so many bases when it comes to gut health and overall liver and pancreas health.
Some other common prokinetics:
- drugs such as prucalopride, itopride, and naltrexone (prescribed by a gastrologist during bacterial eradication)
- natural substances: oil of rosemary, peppermint, thyme in capsule form, iberogast, ginger, or chamomile.
Keep in mind that cleansing before an extended fast is crucial, and understanding laxatives and prokinetics is a good too to have under your belt.
Segmentation and migrating motility complexes & Gastroileal reflex
How to improve the MMC for SIBO AND IBS?
FASTING BETWEEN MEALS
Explained in detail in this post.
ACTIVATE THE VAGUS NERVE
I talk about the parasympathetic nervous system quite a lot. I explain how some proponents of the long covid vagus nerve theory say that brain retraining, meditation, deep breathing, and yoga help their symptoms. I try and repeat this over and over again.
You don't need to become a Buddhist monk to heal or activate your vagus nerve.
Deep ketosis downregulated the sympathetic and upregulates the parasympathetic. Another big win for fasting.
PROKINETIC SUPPORT
Explained pretty well in this post. The takeaway is that using multiple prokinetics can be beneficial as many of them have different mechanisms of action.
TOLERANCE OF HIGH FODMAP PRODUCTS
Explained in this post. If you are improving your MMC and base-level health, you can qualify it by showing an increase in tolerance to high FODMAP foods.
FIXING YOUR DIURNAL RHYTHM
Sleep is the basis of health. It's your job to build a healthy diurnal rhythm that includes waking up and getting enough access to sunlight, as well as sleeping well, not eating before sleep, and letting your brain-gut axis heal.
I support melatonin for emergency uses, but overall you need to stay away from supplements that your body can create itself, lest you damage your pathways.
Finally, Why you should be fasting for IBS and SIBO?
Nothing applies to everybody, that’s definitely a solid rule to keep in mind. Getting this out of the way, you already fast for 7-8 hours when you sleep, so stop being so scared of it.
The Migrating muscle complex gets activated with a 4-hour fast. So let’s get to it. You are already a bit of a faster, since you fast while you sleep.
Start with waiting for breakfast for an hour or two extra, don’t eat a few hours before bed and there you have it, you’ve started your fasting and healing journey.
The benefits of fasting are fantastic. Once you start healing your migrating motor complex, your gut, and your digestive system, you will start to realize that fasting was always there for you, you just didn’t know it. If you have IBS or SIBO and you have never tried to fast, I am trying to convince you that this is the time to try it.
You know that when you don’t eat, so probably in the morning, you feel your best. Extend that feeling. Let your body guide you. Another thing to consider with fasting is that your fat cells have all the nutrients and vitamins you need.
Work on replenishing your fat cells during your refeeds with good healthy foods, and you will exponentially feel better on future fasts as well. Once you are comfortable with intermittent fasting you can work your way up to your first 24 hours fast and longer. This will introduce you to a new world where you can start to wave goodbye to both SIBO and IBS.





