Have you ever had chronic diarrhea? Lots of people have experienced this through various forms of fasting, diet changes, liver flushes, and more. Well, a lot of this has to do with bile when it comes to fasting. Let’s dive deeper into how fasting can affect bile acid in the body.
The paper we’re using today is called: Fasting and refeeding triggers specific changes in bile acid profiles and gut microbiota. One of the more important conclusions of the paper was:
“Bile Acid biosynthesis in liver and intestinal reabsorption were suppressed under fasting status, whereas refeeding ameliorated the decrease in biosynthesis and reabsorption of BAs due to fasting.”
What are bile acids?
Bile acids are a group of molecules produced in the liver from cholesterol. They play a critical role in the digestion and absorption of dietary fats and fat-soluble vitamins (A, D, E, K) in the small intestine. After production, bile acids are stored in the gallbladder and released into the intestines when food is consumed. Here, they act as detergents, emulsifying fats to facilitate their breakdown and absorption.
Bile acids are also key in signaling pathways that regulate their own production, glucose, lipid metabolism, and energy balance. After their action in the intestine, they are mostly reabsorbed back into the bloodstream and returned to the liver for reuse, a process known as enterohepatic circulation. This efficient recycling mechanism allows the body to maintain a consistent bile acid pool with minimal daily synthesis requirements.
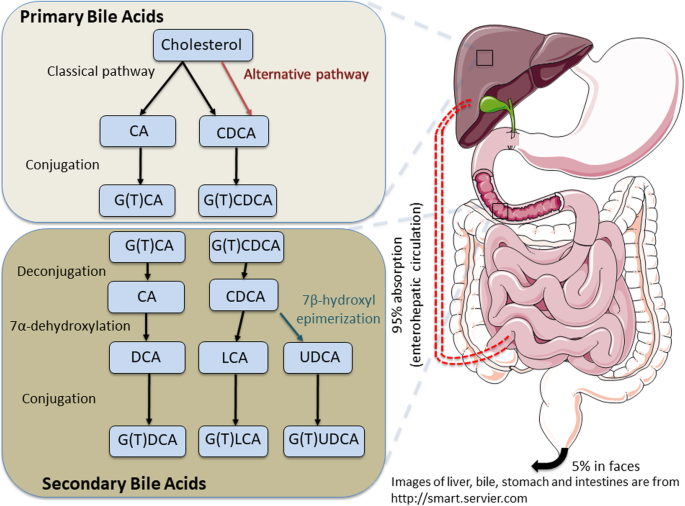
Alterations in bile acid metabolism can lead to digestive issues, liver diseases, and metabolic disorders. Understanding bile acids' roles and regulating their metabolism is crucial for maintaining health.
Bile acids and fasting
Imagine sitting on a toilet with liquid coming out of both sides. Not a pretty sight, nor a pretty feeling. I’ve personally talked to a lot of fasters who fall into this drastic diarrhea situation, and what’s helped most of them is dry fasting with the correct prep and refeed. That means you might need to put away your regular diet when prepping and refeeding. There’s good reasoning for avoiding fat before and after a long fast. You can get away with it only so many times until you’re suddenly hit with diarrhea and need to run to the toilet.
I think it’s important that you are aware of what bile acid signifies. The liver creates the bile and then stores it in the gallbladder. The gallbladder is then “squeezed” when our body sends the signal that fat needs to be digested. Squeeze, squeeze. Well, a few things should come to mind right away. One, we have varying levels of bile acids in the body, which means that we have a set limit to how much fat we can digest at a given time. Makes sense right? Overdo it with a massive meal with too much fat and what happens? Pain and digestive stress. Now, diets play a big role in how well your bile acid production and gallbladder function. Sure, if you eat more and more fat in your meals your body should hopefully adapt to it and increase your baseline amounts. This is similar to working out, you need to keep pushing yourself more and more to get stronger. But you also need to eat the right stuff. If you overdo it right after a fast you might land in the hospital.
Diet and bile acid
Another thing to consider on the topic of bile amounts and bodies ability to use it is diet. If you are more plant-based, your bile production will be lower, your gallbladder will probably be weaker. Weaker does not mean unhealthy in this case. It is simply an adaptation to your diet. Who knows, maybe less work needed from the gallbladder is one of the prerequisites to health or longevity in the long run. Maybe - But I wouldn’t worry about that, since I believe in the power of fasting. However, it is more common to see plant-based dieters get gallstones. What does that mean? Well, if you use fewer bile acids, and the gallbladder isn’t ‘squeezed’ as often, the bile stagnates inside and creates more possibilities of gallstone formation. Look into herbs that stimulate the bile flow, but if you’re worried you might already have gallstones, look into malic acid and citric acid. The easiest way to get it is by drinking lemon water daily, but I also like to take magnesium malate in the morning, or you can look into tart cherry juice too.
Bile acid is a very important aspect of fasting, and it’s one of the reasons behind so many ritualistic preparations. Imagine people planning enemas, liver flushes, malic acid preps, and dietary changes. Even if most people don’t understand the importance of bile in an extended fast, they still follow guidelines and protocols that have inherently built around this issue over many years of trial and error. In a way, this is real-life empirical research.
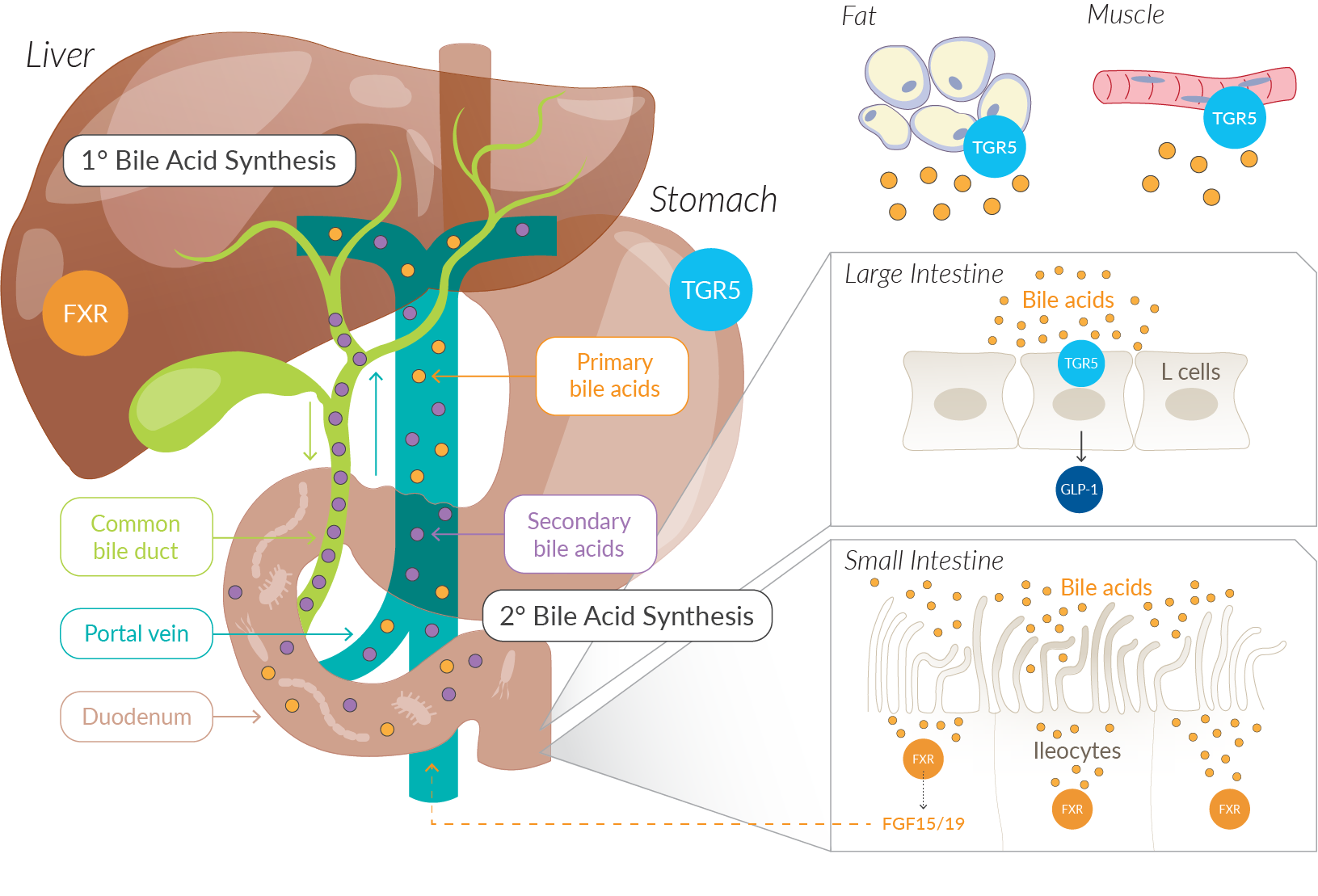
Now zero-carb diets are becoming increasingly popular, and with them, big requirements from your liver and bile system. This doesn’t necessarily mean they are bad, as many people will quickly try to claim. But this also doesn’t mean that they are perfectly safe. We just don't have enough data to make decisive claims. We also need to keep an open mind to body adaptations, especially super fat-adapted bodies. We know there are metabolic shifts like an increase in cholesterol that is directly linked to extra bile acid production. Regardless, we need to tread carefully and appreciate the safety of sticking to tried and true methods that focus on lowering your bile pre-fast and then slowly waking it up afterward. This also creates opportunities for mixing and matching diets. With low-carb diets that prepare you very well for long fasts, followed by diets that are more carb-based. This is valuable if you're looking into alternating between different metabolic states as so many people get stuck in one type of diet which I don't think is ideal for health.
It’s very common to see people abruptly start a long fast and have their bile reabsorption pathways get suppressed and then leading to bile stagnation in the digestive system, pain, and possible complications. Upon restarting, they create drastic bile requirements by ingesting fats. Requirements that cannot be filled by the current empty bile system. This may be beneficial in flushing some remaining bile, but at the same time, it causes digestive distress which will take away from the body’s required energy for healing.
Some people on high-fat diets might run into too much bile flow and have a lot of bile in the stool. This can be caused by your body overreacting to high amounts of fat. This is often also related to a lack of gut bacteria that can conjugate and deconjugate the bile acid, another reason why our microbiome is important. A dry fast can be very curative due to its bile reabsorption suppression and microbiome healing capabilities. Just make sure you refeed with food that promotes a revival of the microbiome, including probiotics like kefir.
Low Bile Acid Consequences
Bile acids play are critical for good fat digestion and absorption. If your bile acids are lacking, you can expect a lot of negative downstream effects, such as loose fatty stools, energy deficits, and vitamin deficiencies. Fat-soluble vitamins require a good fat processing system, and therefore, a good functioning bile acid system is required. Managing bile, avoiding bile stagnation, and giving your body the best possible gentle reawakening is key to healing and thriving after a dry fast.
We have a study on fasting and refeeding and how it affects bile acid profiles. They also looked at gut microbiota, but that information is too vague with little value for us right now. The most important findings were how drastically the microbiome can affect bile acid conjugation and how quickly it can adapt to fasting situations. This means that making the effort to manage bile before and after a dry fast is very important.
What this fasting bile acid study observed

Plasma levels
In the blood we see that there are more bile acids during the refeed than normal, meaning that our body is doing its best to resupply and upregulate bile acid production. This makes sense because during fasting our reabsorption genes are suppressed and that means that we do end up losing quite a bit of bile in our feces. We also see that unconjugated primary bile acid levels plummet during a fast. What does this tell us?
- There is more bile acid volume in the blood during a refeed, around 10% more.
- Indicators that the body is trying to replenish the bile acid levels
- The body stops bile production (unconjugated primary) during a fast very quickly, even during a “short” 24-hour fasting period.
- Getting higher levels of secondary bile acid in the blood indicates that there is extra bile going around and an indication that the altered gut microbiome is still conjugating more bile than normal.
Feces levels
Interestingly we see that nearly the amount of bile that’s found in blood levels when eating normally, we see the same amount by volume, in the feces at the end of a 24-hour fasting period, amazing. Since we almost completely stop producing bile within the first 24-hour hours, it indicates that our gut bacteria will run out of it as an energy source very quickly. It also means that we are draining our bile nutrients. What does this tell us?
- The body dumps bile acid while on a fast. Even a short 24-hour one. This is because of reabsorption suppression.
- The body loses very little bile acids when there is nutrient abundance
- The body's gut bacteria use a lot of bile acids for energy during a 24-hour fast
- The gut bacteria lose bile energy potential drastically after 24 hours (probably why the extra powers of a fast are related to a minimum of 36-hour fasts)
- Refeeding after a fast needs to take into consideration lower amounts of bile acid
- Overfasting can drain micronutrients necessary for bile production, the same way vomiting daily can destroy stomach acid and electrolyte balance.
Additional things to consider when Dry Fasting
Bile reabsorption suppression: The interesting thing we see is that during a fast we start to see a lot of unconjugated bile arriving in the feces, meaning that our body is not absorbing it. This is due to intestinal reabsorption suppression. What does this mean? It means that we can lose a lot of our bile acids due to a fast. We can think of it as bile dumping. It’s a reason why it is common, especially for low-carb eaters to have diarrhea after breaking a fast. This can be a mix of the body not being able to properly reabsorb the bile acids in the ileum (this means that the recycling of bile is affected), and also malabsorption of fat (fatty stools). This can make your stool greasy and more difficult to flush. Have you had that happen to you after a long fast?
This plays a big role in deciding how you should refeed after a fast. If we force fat during the refeed, we are potentially causing unnecessary harm to the body by losing valuable bile salts, and not absorbing the nutrients from the fat. And we know that we NEED nutrients and energy for the intense rebuilding phase. That’s why it’s critical to start the refeed with moderate protein and complex carbohydrates. If you are very anti-carb I understand that you’ll prioritize protein, however, protein is our most inefficient source of energy, so keep that in mind. If you are scared about triggering viral or pathogen responses to high blood sugar, there are other strategies that involve medication or herbs.
Running out of bile acids on frequent fasts: What does this mean for shorter dry fasts or trying to do Dry OMAD type of intermittent fasting? Well, you're going to be constantly in a cycle of stopping bile and restarting it. A dry fast is powerful. Most people liken it to being 3x stronger than a water fast. So we can expect the effects of bile suppression to be 3x stronger too. This means that if you start the fast having come from a regular diet including fat, you’ll have a lot of bile free floating in your system, not being reabsorbed in the ileum because of the suppression, and therefore suffer from a short bile stagnation followed by dumping it with the next bowel movement when you break the fast.
This means that you’re going to keep throwing your liver and bile ecosystem into a stressful loop. Then what? Dry OMAD is not smart, but if you do it, you need to gradually enter and exit. So if you decide to do something like a 36-hour dry once a week, you can surround it with hydration-focused OMAD, which won’t have such a powerful effect as a dry fast, and therefore a weaker bile stagnation/suppression effect. When coming out of even a 36-hour dry fast, you come out of it gently with no fat broth, kefir, and soft veggies, or make sure you have bile salts as a supplement in case you mess up.
Bile overproduction: Sometimes your body might go into an overproduction loop. Often seen with keto-style diets where fat is the main component. If you eat fat too soon you might run into two problems. One, your bile supply has not returned so you will have undigested fat running through your system and into the toilet. This causes digestive stress and discomfort, further diminishing healing by not letting the body rest and digest without stress. Two, you might trigger your body to start overproduction of bile and with it conditions like Bile Acid Malabsorption (BAM) or too much concentrated bile and cholesterol which will create gallstones and give you liver pain.
Ok, so how do you prepare for a liver flush before any type of extended fasting?
How to Prepare for a Long Fast: Bile Health Strategy
- Increase Hydration - Ensures proper hydration to help thin bile and promote its flow. Dry fasting is especially complicated when it comes to bile and bile flow, so handling it as carefully as possible is paramount. Hydration is important, and we don’t want to be in chronic dehydration when we can avoid it. We use dry fasting rarely, and like a surgical knife. Only when needed, and very precise.
- Liver flush - Flushing the liver’s main goal is to remove stagnating bile and with it potential gallstones and other matter. Think of it like CPR on your liver. I don’t believe you need to liver flush for every single fast, but when you’re embarking on really long ones, it’s an important aspect to consider.
- High-Fiber Diet - Fiber-rich foods aid in regular bowel movements and the elimination of bile acids. Before fasting, increasing the intake of dietary fiber can help bind bile acids in the gut, leading to their excretion. This can potentially moderate the pool of bile acids available for alteration during fasting. This strategy helps in preventing bile stagnation, which we do not want during a long fast.
- Reduce Fat Intake - Eases the workload on the gallbladder to prevent bile stagnation during the fast. This is seen with vegan diets prior to the liver flush as well. It’s very common to employ a light vegetarian type of diet pre-fast but there have been lots of success stories coming in from a more ketogenic fat-adapted diet too. It’s a good strategy to reduce bile flow a few days before the fast and that means lower the fat intake.
- Add Lemon Water - Stimulates bile production and supports liver and kidney health. This also reduces kidney stone risk and gallstone risk due to the citric acid. I would also mix in malic acid during the preparation. If you look at my protocols, I prefer to use magnesium malate in the mornings.
Post-Fast: Reactivating Bile Flow and Digestive Health
- Gradual Rehydration - Slowly increase water intake to rehydrate and support bile flow. Most of this is to prevent edema, which is the swelling of cells due to sodium imbalance and high levels of aldosterone. Shocking the system with lots of water further causes an even more drastic swing in sodium levels. These swings can impact the nervous system and cause complications too. You should always approach stress gradually for the best results.
- Light Vegetable Broths - Start with vegetable broths to provide minerals and hydration without overstimulating the digestive system. Light broths will provide very minimal stimulation to bile, allowing the body to rehydrate and reabsorb minerals as a first step to healing, before having to worry about bile. It also won’t overly spike insulin, and
- Add Soluble Fiber - Introduce soluble fiber to bind bile acids and encourage bile production. We want to clean up the intestines from any remaining stagnant bile. We need fiber for this. This is where fiber is going to help. Stagnating bile can also confuse the body and limit the production of fresh new bile. There’s a reason the post-fast diets include oatmeal and buckwheat.
- Incorporate Healthy Fats Slowly - Gradually include healthy fats to stimulate gallbladder and aid in fat digestion. You need to start with the least complex fats and that should include healthy plant fats like coconut fat, olive oil, and avocados. Even then, you should not jump into them too soon after a fast. Then you can slowly begin to scale back up to complex fats. A hack is mixing in a tiny bit of apple cider vinegar with your meal. Some people add a little bit into their broths too.
- Probiotic Foods - Add probiotic foods to help restore gut flora balance and support bile acid metabolism. Incorporating fermented foods into your diet, like yogurt, kefir, and sauerkraut, can introduce beneficial bacteria to the gut, potentially offsetting the fasting-induced decrease in beneficial species. Taking a probiotic supplement before and after fasting may help maintain levels of beneficial bacteria like Lactobacillus and Bifidobacterium, supporting overall gut health.
- Increase Bitter Greens - Continue stimulating bile flow with bitter greens for liver detoxification. Upon refeeding, introduce foods that are known to stimulate bile flow and support liver health, such as beets, artichokes, and leafy greens. These foods can help kick-start the liver's bile acid production and support the re-establishment of normal bile flow.
- Supplements: like taurine, which is involved in the conjugation of bile acids, may help support bile acid metabolism during the fasting preparation phase. Milk thistle and Berberine are known for their liver-protective effects and may also support bile production. TUDCA can be an important supplement if you’re not creating enough bile, and bile salts work too but may not be as effective for some people.
- Add Lemon Water - Stimulates bile production and supports liver and kidney health. This also reduces kidney stone risk and gallstone risk due to the citric acid. I would also mix in malic acid during the preparation. If you look at my protocols, I prefer to use magnesium malate in the mornings.
Bile and Microbiome
Fasting has shown a lot of promise in helping fix liver and gallbladder issues. You just have to remember to refeed gently and correctly. Following established guidelines that have worked for many years is the safest way to go about it. One of these guidelines is that kefir is one of the best refeed foods and preparatory foods available.
There’s a paper called: Kefir Ameliorates Alcohol-Induced Liver Injury Through Modulating Gut Microbiota and Fecal Bile Acid Profile in Mice https://pubmed.ncbi.nlm.nih.gov/37933689/.
Now we start to see a correlation with the Russian Dry Fasting protocols that love to include kefir.
Some things to know about gut bacteria and bile acids:
- Gut bacteria can deconjugate bile acids and send them back into the bile feedback loop
- Eating more fat will trigger more bile and with it a change in bacteria
- Some bacteria can use deconjugated bile for energy
- Long-term alterations in bile acids and gut microbiome can change host metabolism, slowing it down and affecting glucose regulation. You become more adapted to fat burn, and a steadier form of energy, but lose the ability for intense bursts characterized by glucose and glycolysis.
- The bacteria that prefer bile-rich environments are Clostridium, Bacteroides, and some lactobacillus strains.
Final Thoughts
So now we start to see the importance of modulating and taking care of the liver and bile acid production when it comes to fasting and health. It’s not a well-documented field, and it shows when you try to google things like liver and gallbladder issues. You realize that when it comes to health problems surrounding these organs, doctors try different things and have varying success rates. What works for one person doesn’t work for another. Often, people are left to fend for themselves.
Gallbladder removal surgeries are becoming more and more common. This goes to show that in the last few decades, we have started stressing out our bile systems much more. Could it be through seed oils which are extremely unnatural and highly processed? Quite possible. I mean they’re cheap and in so much of the processed food. But even getting rid of all seed oils, something I believe most people searching for a healthy diet are advised to do, may not be enough. You still need to take extra precautions and care for your bile system, especially when it comes to fasting.


